How it unfolded
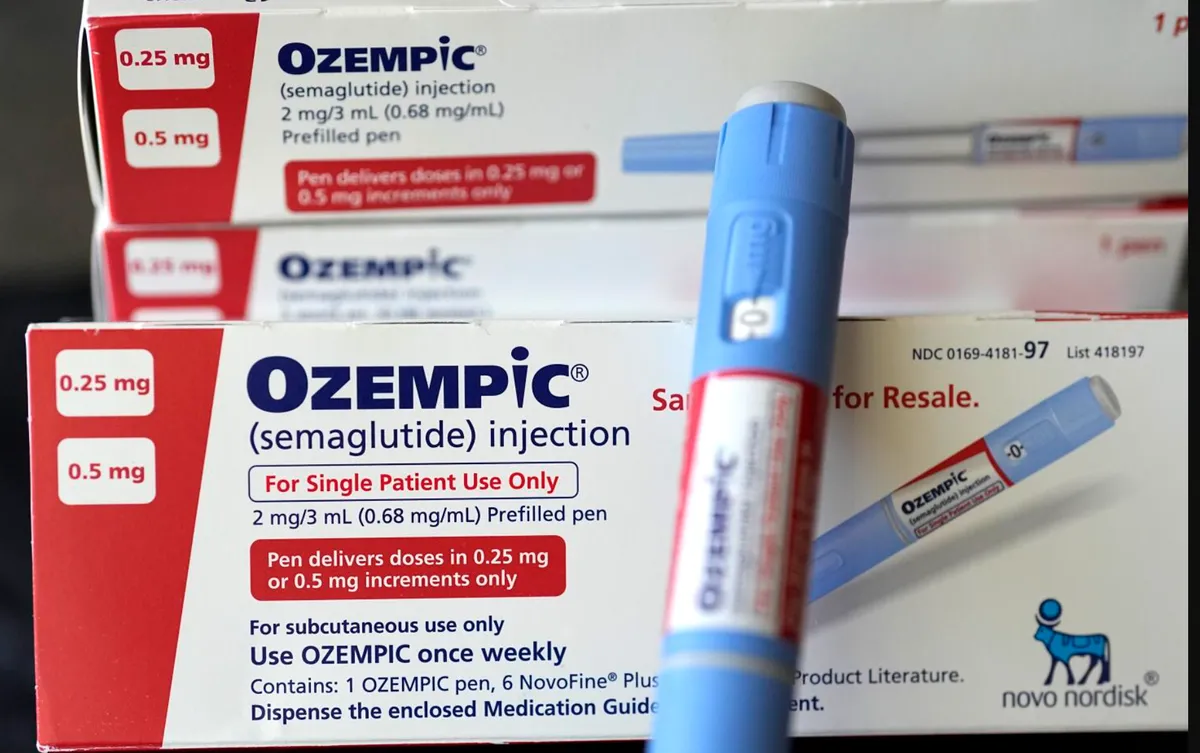
Metformin has been a standard first-line treatment for Type 2 diabetes for more than 60 years, primarily known for its ability to lower blood glucose levels by reducing glucose production in the liver. However, recent research has begun to reveal a more complex interaction between metformin and the brain, particularly through a specific pathway in the ventromedial hypothalamus (VMH).
In groundbreaking studies conducted in 2025, researchers discovered that metformin interacts with a protein called Rap1 within the VMH. This finding marks a significant shift in the understanding of how metformin functions. According to Makoto Fukuda, a leading researcher in the field, “It has been widely accepted that metformin lowers blood glucose levels mainly by reducing glucose production in the liver.” This new evidence suggests that the drug’s effects extend beyond the liver, engaging directly with brain mechanisms.
Experiments in mice demonstrated that metformin is capable of reaching the VMH and deactivating Rap1. When Rap1 was disabled in the forebrain of these mice, they became resistant to the effects of low-dose metformin. Conversely, when Rap1 was activated, glycemia increased, and the drug’s ability to reduce blood glucose levels was hindered. This indicates that the VMH Rap1 pathway is an essential mediator of metformin’s effects.
Furthermore, the activation of SF1 neurons in the brain appears to be crucial for metformin’s antidiabetic effect. Fukuda noted, “We found that SF1 neurons are activated when metformin enters the brain, suggesting that these neurons are directly involved in the way the drug works.” This insight opens up new avenues for understanding how metformin can be optimized for better therapeutic outcomes.
In addition to its primary function of managing blood sugar levels, metformin has been studied for potential benefits beyond diabetes treatment, including effects on brain aging. The implications of these findings are significant, as they may lead to the development of new diabetes treatments that directly target this pathway in the brain. Fukuda stated, “These findings open the door to developing new diabetes treatments that directly target this pathway in the brain.”
Moreover, a study involving 400 postmenopausal women found that those treated with metformin had a 30 percent lower risk of dying before the age of 90 compared to those treated with sulfonylurea, further emphasizing the drug’s potential benefits beyond glucose control.
As research continues to unfold, the current state of understanding regarding metformin’s interaction with the brain is evolving. The discovery of its effects on the VMH and Rap1 pathway not only enhances the scientific community’s grasp of diabetes treatment but also raises important questions about the broader implications for brain health and aging. Details remain unconfirmed, but the trajectory of this research could redefine treatment protocols for Type 2 diabetes and related conditions.